Sometimes an arteriovenous malformation (AVM) is found “incidentally,” meaning that it hasn’t caused any symptoms but is found during a CT or MRI scan performed for another reason (for example, after an accident or injury). In those cases, it may not need to be treated at all — in an otherwise healthy patient an asymptomatic AVM may be monitored, but not treated. A neurosurgeon evaluating the diagnostic angiogram will discuss treatment options with the patient and make a recommendation based on the risk of a rupture or other complications balanced against the risks of surgical intervention. The recommended treatment plan will be based not only on the angiogram but also on the patient's clinical history, age, symptoms, and a physical examination. For example, an older patient at low risk for bleed might be advised to have the AVM monitored rather than treated.
The decision to treat a cerebral AVM depends on its location, the risk of future complications if it is left untreated, and the risk of neurological deficits that may be associated with its treatment. Since an arteriovenous malformation is a highly complex condition, it is best treated by experienced neurosurgeons at a high-volume major medical center specializing in complicated cases. At Weill Cornell Medicine Neurological Surgery our team of neurologists, interventional neuroradiologists, neurosurgeons, and radiosurgery specialists have expertise in the evaluation and treatment of AVMs, providing internationally recognized care. See commentary from Dr. Knopman and Dr. Stieg for The Lancet on the management of AVMs.
There are a variety of surgical techniques, which may be used alone or in combination, for the treatment of AVMs. Some AVMs will require just one of these therapies and others will require a combination. Treatments include:
Stereotactic Radiosurgery
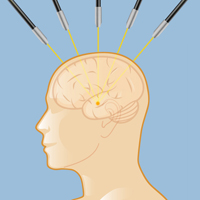
Stereotactic radiosurgery for an arteriovenous malformation consists of highly targeted radiation beams directed at the AVM from multiple angles.
Without entering the skull, neurological surgeons can use stereotactic radiosurgery (highly targeted radiation beams from multiple angles) to treat an AVM. This technique, generally used for smaller AVMs, is effective in up to 80 percent of patients. Radiosurgery is usually delivered in an outpatient setting in a single treatment. The radiation, once delivered, produces a slow narrowing of the abnormal blood vessels over one to three years, until the AVM is obliterated. This is a rapidly developing technique that requires special expertise from a neurosurgeon specially trained in radiosurgery and utilizing the most sophisticated equipment — such as the Gamma Knife, CyberKnife, proton beams, and linear accelerators. Stereotactic radiosurgery is usually only available in major medical centers (see Doctors Who Treat AVMs).
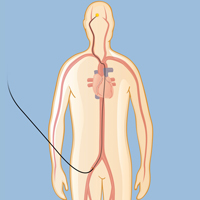
Embolization starts with a tiny catheter inserted into the upper leg and threaded up to the site of the AVM.
Embolization
Another surgical approach to AVMs is endovascular embolization, which involves the insertion of a catheter, or small plastic tube, through an artery in the upper leg or wrist. The tube is guided up the circulatory system to the site of the AVM, where it delivers a liquid “glue" that embolizes or blocks blood flow to the malformed vessels, thus restoring normal circulation. In most cases, embolization alone is not enough to cure an AVM, but it is very useful to reduce the size of an AVM before surgery.In some cases it may reduce a large AVM enough to make radiosurgery a viable option, thus avoiding the need for surgical resection.
Microsurgical Resection
Microsurgical resection of an AVM is open surgery in which the neurosurgeon removes part of the skull to gain access to the abnormal vessels, which are then repaired or removed. In cases where the risk of a hemorrhage is high, or the AVM’s location is inaccessible to an embolization catheter, this surgery may be a patient’s only option. Following this procedure, close monitoring and strict control of blood pressure are required, as well as a high-quality angiogram to determine that the AVM has been completely removed. There are risks involved in any brain surgery, including infection and neurological impairment, but a successful surgical resection that completely removes an AVM virtually eliminates the risk of a future rupture. At Weill Cornell Medicine Neurological Surgery we have a dedicated operating room with angiography equipment, which allows neurosurgeons access to high-tech images to confirm the complete resection of the AVM at the time of surgery.
After surgery, radiosurgery, or embolization, your medical team will monitor your progress and conduct tests to evaluate the success of your therapy.
At Weill Cornell Medicine Neurological Surgery, we understand that being diagnosed and treated for an AVM can be both physically and emotionally challenging. We believe that the trust and cooperation built up over the weeks leading up to the surgery is an important part of recovery. Throughout your journey, we will make decisions together to provide you with the most advanced treatments and the best possible quality of life. Use our online form to request an appointment for an evaluation or a second opinion.
Reviewed by: Justin Schwarz, MD
Last reviewed/last updated: March 2024
Illustrations by Thom Graves, CMI